 Cerebrovascular Accident (CVA)
Cerebrovascular Accident (CVA)
A CVA, commonly known as a Stroke, is a complex neurological dysfunction that is caused by a lesion in the brain.
The following charts will review the causes and symptoms of CVA, as well as occupational therapy treatment methods.
| Type | Presentation | Risk Factors | Photo |
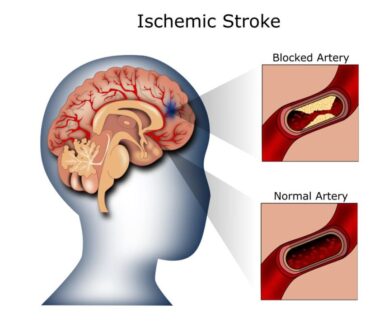
| Ischemic | An embolism in the brain blocks blood flow to brain tissue, causing ischemia or lack of oxygen to brain tissue. | Non-modifiable: age, gender, ethnicity, heredity Modifiable: hypertension, cardiac disease, diabetes and glucose metabolism, cigarette smoking, excessive use of alcohol, use of illegal drugs, obesity, diet and exercise, emotional stress |
 |
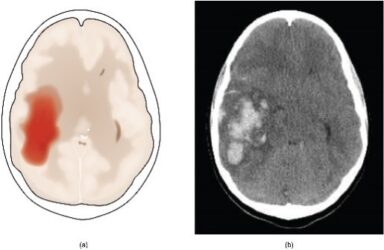
| Hemorrhagic | A blood vessel in the brain bursts, causing blood to pool in part of the brain and interrupting blood flow to other parts of the brain. -Subarachnoid – an aneurysm near the surface of the brain bursts and blood leaks out in the space between the skull and the brain. -Intracerebral hemorrhage – a blood vessel inside the brain ruptures and blood leaks out into the brain tissue.-deep hypertensive intracerebral hemorrhage – involves ruptured saccular aneurysms, bleeding malformations, or spontaneous lobar hemorrhages. |
Non-modifiable: arteriovenous malformation (AVM), aneurysm, age. Modifiable: high blood pressure, cigarette smoking, use of oral contraceptives, excessive alcohol intake, use of illegal drugs. |
 |
| Transient ischemic attack (TIA) | Brief interruption of blood flow to the brain, causing mild, isolated symptoms that may be repetitive in nature. -duration from a few minutes to several hours -symptoms clear completely -may be a warning sign of an impending larger ischemic attack |
Atherosclerotic disease | 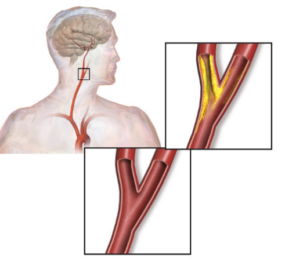 |
The symptoms resulting from a CVA differ, depending on the location of the CVA.
This chart reviews symptoms that are associated with the different arteries of the brain.
| Artery | Location Supplied | Symptoms | Video Example |
| Internal carotid artery | -One of the primary arteries to the brain. -Part of the Circle of Willis, off of which other arteries branch. |
1. Contralateral hemiplegia, hemianesthesia. And homonymous Hemianopsia
2. Occurrence in dominant hemisphere is associated with aphasia, agraphia/dysgraphia, acalculia/dyscalculia, right/left confusion, finger agnosia 3. Occurrence in non-dominant hemisphere associated with perceptual dysfunction, unilateral neglect, anosognosia attention deficits, loss of topographic memory |
|
| Middle Cerebral Artery -most common location of CVA |
-Largest branch of the internal carotid artery -Supplies a portion of the frontal lobes, lateral surface of the temporal and parietal lobes. |
1. Contralateral hemiplegia with greater involvement of the arm, face and tongue; sensory deficits; contralateral homonymous hemianopsia and aphasia if the lesion is in the dominant hemisphere
2. Pronounced deviation of the head and neck toward the side of the lesion 3. Perceptual deficits such as anosognosia, unilateral neglect, impaired vertical perception, visual spatial deficits |
|
| Anterior Cerebral Artery | Supplies the frontal lobes. | 1. Contralateral lower extremity weakness, more severe than upper extremity weakness.
2. Apraxia, mental changes, primitive reflexes and bowel/bladder incontinence may be present. 3. Cortical sensory loss in lower extremity. 4. Intellectual changes including confusion, disorientation, whispering, slow processing speed, distractibility, limited verbalizations, amnesia 5. Total occlusion of artery results in contralateral hemiplegia with severe weakness of the face, tongue and proximal arm muscles, marked spastic paralysis of the distal lower extremity. |
|
| Posterior Cerebral Artery | Supplies the temporal and occipital lobes of the left cerebral hemisphere and the right hemisphere. Also supplies the brainstem. | 1. Broad, multiple symptoms
2. Sensory motor deficits, involuntary movement disorders, postural tremors, hemiataxia, memory loss, astereognosis, dysesthesia, kinesthesia, contralateral homonymous hemianopsia, anomia, topographic disorientation, visual agnosia |
|
| Cerebellar Arteries | Supply the cerebellum | 1. Ipsilateral ataxia, contralateral loss of sensation of pain and temperature
2. Ipsilateral facial analgesia 3. Dysphagia, dysarthria, nystagmus and contralateral hemiparesis |
1. Specific treatment is dependent on the type and location of CVA.
2. Early medical intervention
-maintain open airway
-hydration with intravenous fluids
-treatment of hypertension
3. Ongoing prevention of deep vein thrombosis (DVT) in the lower extremities due to prolonged bed rest
-clots can dislodge and travel to the lungs, causing pulmonary embolism which can be fatal.
4. Complications may include pneumonia, cardiac disease.
5. In addition to symptoms listed above, symptoms may include low-grade fever, lethargy, bowel/bladder dysfunction.
6. CT or MRI scans evaluate the cause and location of CVA.
7. Once medically stabilized, the condition is not progressive.
8. The first 3 to 6 months after CVA is the most crucial time for improvement.
1. Recipients of occupational therapy are qualified to make decisions about their occupational functioning and should be allowed to do so.
2. Patients should be given an active role in defining goals and desired outcomes.
3. The focus of treatment should be contexts in which the patient lives, including their roles, interests and culture.
4. The patient is the problem definer and solver. Patients should be allowed to set personal goals and evaluate performance.
| Name of Test | Type of Test | Areas Measured | Video Example |
| Canadian Occupational Performance Measure | Semi-structured interview | Daily occupations of importance, including self care, productivity and leisure -patient rates both performance and satisfaction in each area -insures that the patient is an active participant in the rehabilitation process |
An occupational therapist uses the COPM to interview her 95 year old grandmother. |
| Arnadottir Occupational Therapy Neurobehavioral Evaluation (A-ONE) | Structured observation | Affect of dysfunction on BADLS and mobility tasks. | LINK: Website that provides information about the A-ONE. |
| Assessment of Motor and Process Skills (AMPS) | Standardized observational assessment | Evaluation of motor and process skills and their effect on IADLs. | A brief introduction to the AMPS and samples of test administration. |
| Kohlman Evaluation of Living Skills | Standardized test | Evaluation of 17 BADL and IADL skill areas. | An occupational therapy student administers the KELS to an elderly man. |
| NIH Stroke Scale | Observational rating scale | Rates 15 neurological symptoms to determine severity of CVA | Demo of administration of the NIH Stroke Scale with an elderly patient. |
| Barthel Index | Observational rating scale | Rates BADLS and mobility, including bowel, bladder, feeding, grooming, dressing, transfer, toileting, mobility, stairs, bathing | An occupational therapist demonstrates administration of the Barthel Index with an elderly woman who has returned home following a CVA. |
……..
| Type of Occupation | Problems | Treatment Techniques | Examples | Video |
| Occupations while seated
|
1. Loss of trunk and postural control
2. Inability to sit in proper alignment 3. Loss of righting and equilibrium reactions 4. Increased risk for falls 5. Dysfunction in limb control 6. Visual dysfunction secondary to head and neck misalignment 7. Symptoms of dysphagia due to misalignment 8. Impaired ability to interact with the environment 9. Decreased ADLs |
1. Establish a neutral yet active starting alignment -feet flat on floor in weight bearing position -equal weight distribution through ischial tuberosities -neutral to slight anterior pelvic tilt -erect spine -head over shoulders and shoulders over hips 2. Establish the ability to maintain the trunk in midline using external cues. -mirror for visual feedback -verbal cues -environmental cues 3. Maintain trunk ROM through wheelchair and armchair positioning that maintains the trunk in proper alignment. -exercise program focused on trunk ROM -hands on facilitation as needed for mobilization 4. Dynamic weight shifting activities to allow practice of weight shift through the pelvis. -set up occupations to reach beyond arm span and limits of stability -adjust posture.. 5. Trunk strengthening -use tasks that require the patient to control the trunk against gravity -bridge the hips in supine position to strengthen the back extensors 6. Compensatory strategies and environmental adaptations -use when trunk control does not improve to a sufficient level, putting patient at risk -compensatory strategies such as one-handed shoe tying -adaptive equipment, including reachers and long handled devices -wheelchair seating systems -lumbar rolls -lateral supports -cushions |
1. An occupational therapist positions a man who has had a CVA in upright sitting on the edge of a mat table and asks him to reach for cones with his unaffected arm, positioning the cones just beyond the man’s reach and forcing him to use his trunk muscles while he shifts his weight.
2. An occupational therapist positions a man who has had a CVA in sitting with mild lateral support to allow him to perform upper extremity pulley exercises using a grip assist mitt on the affected hand. 3. An occupational therapist facilitates corrections to posture in a woman who has had a CVA while she completes grooming and hygiene tasks. |
|
| Occupations while standing
|
1. Asymmetrical weight distribution -weight distribution is seen through the lower extremities as well as the trunk .. 2. Automatic postural controls may be impaired. -ankle strategies, used to maintain center of mass and control small, slow, swaying motions -hip strategies, used to maintain or restore equilibrium -stepping strategies, used when ankle and hip strategies are ineffective .. 3. Resulting problems with base of support (BOS) -movement of BOS toward the COM -steps taken to widen BOS |
1. Establish symmetrical BOS and proper alignment to prepare to engage in occupations -hands on support as needed -feet approximately hip width apart -equal weight bearing through feet -neutral pelvis -knees slightly bent -aligned and symmetrical trunk .. 2. Focus on ability to bear weight and shift weight through affected lower extremity. .. 3. Encourage dynamic reaching activities in multiple environments to develop task specific weight shifting abilities .. 4. Use the environment to grade task difficulty and provide external support5. Train upright control within the context of functional tasks |
1. An occupational therapist provides contact guard support to a woman who has had a CVA. The therapist facilitates small weight shifts as the woman stands next to her kitchen counter and uses both hands to transfer plates from her kitchen table to the cupboard.
2. An occupational therapist teaches a woman who has had a CVA to compensate for her affected leg while side-stepping to allow her to sweep the floor. |
|
| Inability to use language
|
Aphasia – a language disorder that results from neurological impairment
Global aphasia Broca’s Aphasia Wernicke’s Aphasia Anomic aphasia – difficulty with word retrieval |
1. Give the patient time to respond – do not force a response .. 2. Use concise language and simple sentences .. 3. Insure generalization, or transfer of learning from one context to another -vary treatment environments -vary the nature of tasks -help patient to become aware of how he or she processes information -teach processing strategies -relate new learning to old .. 4. Types of transfer i. Near transfer – involves transfer of learning between two tasks with one or two different characteristics iii. Far transfer – involves transfer of learning between tasks that are conceptually similar but few or no characteristics in common iv. Very far transfer– spontaneous application of learning to everyday living |
1. A woman who has had a CVA uses adaptive techniques that she learned in the inpatient therapy clinic to transfer from her wheelchair to the toilet in her bathroom at home. .. 2. A man who has had a CVA with resulting Broca’s Aphasia uses an app on an iPad to communicate with his family. |
|
| Inability to use upper extremities
|
1. Limitations due to: -pain -contracture -loss of motor control -weakness -learned disuse .. 2. Subluxation:-malalignment of the shoulder caused by instability of the glenohumeral joint -common complication of CVA -inferior subluxation – head of the humerus slides below the glenoid fossa – caused by muscle weakness and atrophy -anterior subluxation – head of the humerus sits anterior to the glenoid fossa – caused by weak rotator cuff musculature and muscle spasticity -superior subluxation – head of the humerus lodges under the acromion process and the coracoacromial ligament – also called high riding shoulder … 3. Tonicity: -low muscle tone immediately following CVA -glenohumeral joint and wrist are susceptible to damage due to subluxation and unstable wrist -splinting used to maintain joint alignment, protect tissues from changes in length, prevent injury, and assist with edema control -resting hand position to provide support to the palmar arch while maintaining neutral wrist position -high muscle tone may develop several days or weeks after CVA, resulting in limited movement and/or contracture of the affected arm |
1. Evaluation should focus on assessing the patient’s ability to integrate UE performance of functional tasks -use the affected UE to support performance … 2. Standardized assessments include TEMPA, AMAT, Jebsen, AMPS … 3. Weight bearing through affected UE … 4. Moving objects across a work surface with a static grasp -ironing, opening drawers, polishing furniture … 5. Reaching and manipulation -reach for and hold object -manipulate the object with thumb and finger movements -use objects of different sizes and shapes to facilitate hand control during reach and manipulation -choose activities appropriate for motor control level and grade tasks … 6. Constraint-induced movement therapy (CIMT) -restrain the unaffected arm to force movement of the affected arm … 7. Train the arm to be used in weight bearing while reaching |
1. An occupational therapist assists a man who has had a CVA in pushing a weighted sanding box across the surface of a table using both hands, with the affected hand strapped to the box handle using a grip assist mitt. … 2. An occupational therapist has a woman who has had a CVA stand and hold a box of pegs in her unaffected hand while placing them into a pegboard using her affected hand. … 3. An occupational therapist uses taping techniques to support the affected shoulder of a man who has had a CVA to reduce subluxation in the glenohumeral joint. … 4. An occupational therapist fits a man who has had a CVA with a resting ball splint to provide support to the palmar arch, wrist, and fingers. |
|
 QUICK LINK TO NEURO TREATMENT APPROACHES (Worksheet in Module 4)
QUICK LINK TO NEURO TREATMENT APPROACHES (Worksheet in Module 4)