Alzheimer’s Disease
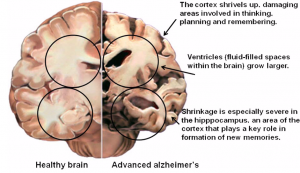

Although the terms Alzheimer’s and Dementia are often used interchangeably, Alzheimer’s disease and dementia are two different terms.
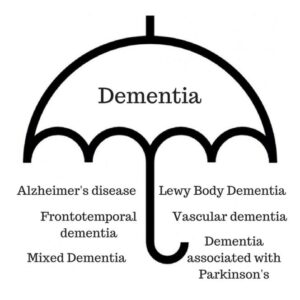
Dementia is an umbrella term. There are many different forms of dementia e.g. Alzheimer’s disease, vascular dementia, dementia with Lewy bodies, and frontotemporal dementia.
ALZHEIMER’S DISEASE IS THE MOST COMMON FORM OF DEMENTIA.
Alzheimer’s disease (AD) is a progressive disorder that causes brain cells to degenerate and die. Alzheimer’s disease is the most common cause of dementia and is characterized by a continuous decline in thinking, behavioral and social skills that disrupts a person’s ability to function independently. The early signs of the disease may be forgetting recent events or conversations. As the disease progresses, a person with Alzheimer’s disease will develop severe memory impairment and lose the ability to carry out everyday tasks.
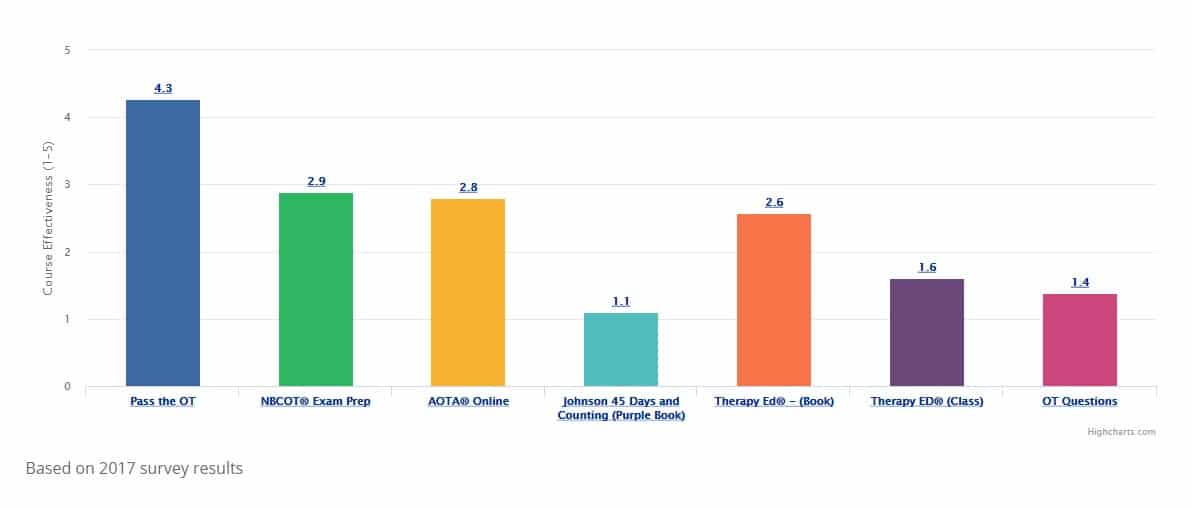
While a number of scales exist, one of the most widely used instruments to stage the course of Alzheimer’s disease is The Global Deterioration Scale for Primary Degenerative Dementia which was developed by Dr Barry Reisberg.
Dr Reisberg, was the first person to describe many of the most important symptoms of AD and the characteristic clinical course of AD. His staging tools are presently governmentally mandated measures throughout the U.S., and widely used worldwide.
** The Global Deterioration Scale for Primary Degenerative Dementia is also referred to as the GDS and the Reisberg Scale.*
THE REISBERG SCALE
The Reisberg Scale is a 7 stage rating scale in which:
Stage 1 reflects no cognitive decline
Stage 2 reflects very mild cognitive decline
Stages 3-7 are defined, respectively, as mild, moderate, moderately severe, severe, and very severe cognitive decline.
The chart below is an overview of the 7 stages of the Reisberg Scale
Stage 1
|
NO MEMORY DECLINE No problems with memory |
| Stage 2 | MILD Memory problems (forgetting keys, wallet etc.) No impact on social life |
| Stage 3 | MILD Others begin to notice memory problems Increased forgetfulness Denies having a problem |
| Stage 4 | CLEAR-CUT DEFICITS Orientated to time and place Difficulty with sequencing/planning Denial At home IADL deficits |
| Stage 5 | MOD-SEVERE DECLINE Cannot live alone Requires cues and assistance Forgets address and phone numbers Disorientated to time and space Inability to drive |
| Stage 6 | SEVERE Irritable Obsessive/delusional Incontinent Incomplete sentences |
| Stage 7 | VERY SEVERE Cannot sit, stand walk or talk At risk for falls, infections and diseases |
The chart below reviews the 7 stages of The Reisberg Scale in detail.
| Stage | Symptoms | Treatment Examples | Video |
| Stage 1
No impairment (normal function) |
The person does not experience any memory problems. Does not show any evidence of symptoms of dementia. | No treatment required | Normal function |
| Stage 2
Very mild cognitive decline May be normal age-related changes or earliest signs of Alzheimer’s disease. |
The person may feel as if he or she is having memory lapses. -forgets familiar words -forgets the location of everyday objects. No symptoms of dementia can be detected during a medical examination or by friends, family or co-workers. |
Cognitive evaluation to determine level of functional impairment.
Recommendations for adaptations to compensate for higher level problem solving and organizational skills. Evaluation and treatment of physical conditions that may be affecting cognitive status. |
A doctor explains the symptoms of mild to moderate Alzheimer’s disease. |