Addressing Sexuality in
Occupational Therapy



Over 30 years ago, the American Occupational Therapy Association recognized sexuality as an activity of daily living, establishing it a rehabilitation priority. Sexuality is an ADL that plays an important part in an individual’s life. Sexuality and sexual participation are common concerns for individuals with disability and chronic illnesses. Research has shown that sexuality and concerns with sexual participation after a disability can impact an individual’s quality of life and self-esteem.
Research has shown that patients expect their health care professionals to bring up the topic of sexuality, and complain of the lack of opportunity to ask questions about their sexual concerns, feel ashamed or embarrassed about the topic of sexuality, do not know which provider is appropriate to answer their questions, and/or they may not feel optimistic about the outcome of such a discussion. On the other hand, health care professionals are often reluctant discuss sexuality because of deficits in knowledge and communication skills, unrealistic fear of offending the patient, and discomfort in asking and addressing sexual concerns. For these reasons, it is important to have a comprehensive view of sexuality in the rehabilitation setting. The key to successful rehabilitation is the willingness to address sexual issues. There is no excuse for ignoring or sidestepping this important part of life after an illness or injury, as has been the practice in the past. Improvement in sexual function and dealing with issues that interfere with sexual abilities have been shown to improve the QOL for individuals with injuries.
As health care professionals, occupational therapy practitioners are well equipped to address sexual participation and sexuality with patients to maximize engagement and satisfaction. OT entails client-centered and occupation-based interventions that maximize engagement and participation in meaningful ADLs. The effects of an illness or disability on the ability to participate in sexual activity can be addressed with occupational therapy intervention. Occupational Therapy practitioners are in an excellent position to normalize sexual health as part of rehabilitation and assist in specifics for sexual activity, such as adaptive sexual devices, environmental controls, and adapted clothing.
SEXUAL REHABILITATION FRAMEWORK
The Sexual Rehabilitation Framework (SRF) is utilized for identifying sexual areas that need attention and for categorizing the severity of sexual issues, according to the priorities of the person with the disability or chronic illness. This framework is applicable for any acute or chronic illness/condition/surgery or disability. In its simplest form, the SRF can be utilized as a checklist that covers the different areas of sexuality and notes how one area can affect another area.
The SRF is contextualized within the 3 principles of sexual rehabilitation:
1. Maximize the remaining capacities of the total body before relying on medications or aids (learning new body maps, breathing, visualization methods, mindfulness exercises)
2. Adapt to residual limitations by utilizing specialized therapies (use of vibrators, mobility devices, training aids, vacuum device aids)
3. Stay open to rehabilitative efforts and new forms of sexual stimulation, with a positive and optimistic outlook
Components of the SRF
1. Sexual drive or sexual interest
2. Sexual functioning abilities
3. Fertility and contraception concerns
Issues about fertility (conception) include the ability to enter into the act of vaginal sexual intercourse with adequate erection and/or to ejaculate with sexual activity, having a normal hormonal milieu in both sexes, and the ability to carry a pregnancy to term and/or undergo labor and delivery with any expected complications.
4. Factors associated with the condition
Medication or other iatrogenic treatments can directly affect sexual function. The patients’ ability to be independent in personal and hygienic care can also affect their sexuality and sexual self-view. Comorbid conditions or conditions such as diabetes that existed before the illness or injury can cause or exacerbate any sexual problem.
5. Motor and sensory influences
Motor function includes the ability to undress independently; to get into a bed or other sexual environment; to reposition oneself or one’s partner; and to touch, caress, and hold a partner. The patients’ ability to transfer or turn independently in bed should be assessed. Spasm and other motor problems can limit the options for sexual activity or participation in the use of sexual aids. Assistive devices to hold sexual aids can be made by therapists. Loss of mobility and dependency on wheelchairs or mobility aids can also limit access to certain social venues and opportunities.
6. Bowel and bladder issues – concern about bladder and/or bowel incontinence during sexual activity is very common
7. Sexual self-view and self-esteem – Body image and sense of attractiveness can be threatened by altered body composition, loss of hair or skin changes, weight loss or gain, obvious bladder and bowel management devices, medication side effects, or use of motor aids or wheelchairs. In a relationship, gender roles can be undermined if there is role change or reversal or loss of independence in daily living, which indirectly affects sexual self-view.
8. Partnership issues – Issues related to the loss of attractiveness and accessibility to social situations and whether the sexual partner also looks after the basic physical or hygienic needs of person (the “caregiver-lover” syndrome) needs to be identified. The ways that people can meet need to be explored, including barriers to and optimizing access. The extensive use of social media and the potential for abuse for all vulnerable populations also should be discussed.
THE PLISSIT MODEL
The PLISSIT model is used by health care practitioners to guide interventions related to patient sexuality and sexual health care needs. The PLISSIT model was developed by Annon (1976) and is an acronym that signifies four levels of intervention: Permission, Limited Information, Specific Suggestions, and Intensive Therapy. The Ex-PLISSIT developed by Taylor and Davis (2006), l is a not linear like the original, but cyclical in nature, with additions of reflection and review. The addition of reflection and review allows the clinician to increase self-awareness by challenging assumptions. The Ex-PLISSIT model also states that all intervention levels should begin with permission-giving.

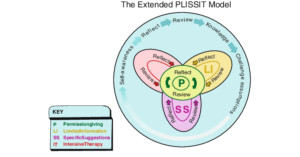
o P– permission which requires the therapist to create an atmosphere which gives the individual permission to raise concerns about his/her sexuality and sexual activity/ies
o LI– limited information that is provided by the therapist to ensure that the individual has accurate knowledge about his/her sexual abilities and potential
o SS– specific suggestions that are provided by the therapist to facilitate the individual’s pursuit of satisfying sexual expression, either alone or with a partner
o IT– intensive therapy which is indicated when the individual requires intervention for long-standing relationship problems and/or enduring sexual problems
TREATMENT APPROACHES
There are three common types of treatment approaches that can be used when addressing sexuality (AOTA, 2013):
1. Health promotion
2. Remediation
3. Modification
Health Promotion
Health promotion involves providing education to at-risk populations (e.g., safe sex practices for clients who are at a high risk for sexually transmitted diseases or unwanted pregnancies).
Remediation
Remediation requires the restoration of “skills such as range of motion, strength, endurance, effective communication, and social engagement as part of meeting sexual needs”. OT Practitioners can work on the individual client factors that are required to engage in sexual activity or increase satisfaction with their sexuality.
Some examples include:
• Increasing strength and range of motion after carpal tunnel surgery so a client can fully weight bear during sex without pain or loss of sensation
• Increasing endurance to maximize sexual participation
• Practicing asking people out to reduce anxiety during social events
Modification
Modification includes “changing the environment or routine to allow for sexual activity” and satisfaction (AOTA, 2013). Positioning and adaptive techniques and tools are included in this type of intervention.
Some examples include:
• Lubrication to reverse the adverse effects of vaginal dryness
• Positioning devices to maximize safety and promote independence with maintaining positions
• Promoting energy conservation techniques to compensate for chronic fatigue
• Information on using personal pleasure devices to engage in self-pleasure
• Modified positions to compensate for activity limitations or restrictions
• Promoting intimacy in place of sexual intercourse
ADDRESSING SEXUALITY DURING ILLNESS OR INJURY
Most chronic and traumatic illnesses have some impact on clients’ sexuality, however, the severity will vary.
Cardiopulmonary Rehab
• Phase 1- inpatient rehab/hospitalization stage
o Tx- *must have a regular pulse and heart rate of 100 or less; patient education (of disease, energy conservation, work simplification, METs), ADLs, decrease anxiety, smoking/dietary modifications, breathing exercises; activities begin at MET level 1-2 and gradually increase to 3.5 (where they then move to next phase of rehab)
• AVOID– isometric muscle work, straining, breath holding, over head exercises (or holding over for extended periods), lateral arm movements/exercises that stretch chest, sexual activity (not until MET level 5-6 is reached) Major depressive episode- 2 week period of depressed mood or loss of interest or pleasure
o Symptoms (5+)- depressed mood most of the day, markedly diminished interest/pleasure, weight loss/gain with increase/decrease in appetite, insomnia/hypersomnia, psychomotor retardation/agitation, fatigue with loss of energy, feelings of worthlessness or guilt, diminished ability to concentrate/make decisions, recurrent thoughts of death/suicide (with or without a plan) and possible attempt
o Possible medication side effects- nausea, headache, sexual dysfunction, insomnia, dry mouth, blurred vision, sedation, postural hypotension, hypertension, anxiety, dizziness, nervousness, weight gain, sweating (possible need for MAOI diet due to meds)
SCI
• Education is essential for the person and part of the ADLs
• Lack of sensation over one part of the body is accompanied by increased or altered sensation over other parts
• Sexual response of the body after SCI needs to be explored
• Viability of sperm in men with SCI is frequently decreased
• Women: changes in vagina lubrication during sex
o Can conceive and give birth
• Special attention when pregnant due to meds and possible clots, auto dysreflexia
o Birth control pills associated with blood clots
o Intrauterine is not recommended and diaphragms may be difficult to position due to loss of sensation in vagina or decreased hand function
o Condom best way
• Sexual activity is an area of occupation
o ADL: functional mobility, personal device care, sexual activity
o Social participation: engaging in desired sexual participation
Chronic pain
Chronic pain is counterintuitive to relaxation, and pain (and the medications used to treat it) can be a serious sexual deterrent for the affected patient and their partner. Anxiety around sexual avoidance can exacerbate the pain or lead to sexual performance anxiety.
Cognitive Impairments
Assertiveness training, training in safe sex, sex education, family/caregiver education
Resources:
https://www.aota.org/~/media/Corporate/Files/Publications/CE-Articles/CE-Article-May-2017.pdf
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5340509/