The Patient-Driven Payment Model (PDPM)

The Patient-Driven Payment Model came into effect October 1, 2019.
The Centers for Medicare & Medicaid Services (CMS) has changed how skilled nursing facilities (SNFs) will be paid for Medicare Part A services. This change impacts how physical and occupational therapy and speech-language pathology services will be reimbursed and could impact how providers furnish therapy.
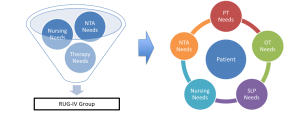
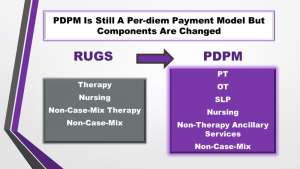
Since 1998, SNFs have been paid under the resource utilization group prospective payment system (RUG-IV PPS). Under RUG-IV, therapy payments are based on the number of days and minutes of services under a single component. RUG-IV includes six therapy payment levels: Ultra-High, Very-High, High, Medium, Low, and Therapy Non-Case Mix.
For dates of service beginning Oct. 1, 2019, providers will receive Medicare Part A per-diem payments under a newly established patient driven payment model (PDPM) resident classification system. Under PDPM, there will be separate per-diem payment rates for PT, OT, and SLP services.
Since the PDPM rule was announced in August 2018, AOTA has been working to mitigate its effects on occupational therapy.
Take note:
1. Groups are NOT mandated. CMS supports practitioners’ clinical judgment regarding the mode of therapy utilized with each patient.
2. Patient outcomes are extremely important and can impact reimbursement. AOTA has created an evaluation checklist to demonstrate the distinct value of occupational therapy in achieving these outcomes.
3. At the urging of AOTA and other organizations, CMS has been very clear that they are watching staffing levels and patient outcomes closely under PDPM. CMS will be monitoring therapy service provision under PDPM, both in terms of intensity and the manner of delivery, at the national, regional, state, and facility levels. Significant changes in the amount of therapy provided to SNF patients under PDPM, as compared to RUG-IV, or the manner in which it is delivered, may trigger additional program reviews and potential policy changes.
https://www.aota.org/Practice/Manage/value/Skilled-Nursing-Facilities-Patient-Driven-Payment.aspx
https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/SNFPPS/Downloads/PDPM-101_Final.pdf