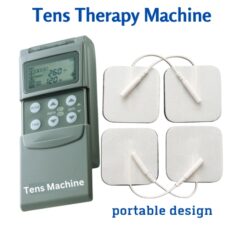
Physical Agent Modalities (PAMs)

Physical agent modalities are those procedures and interventions that are systematically applied to modify specific client factors when neurological, musculoskeletal, or skin conditions are present that may be limiting occupational performance. PAMs use various forms of energy to modulate pain, modify tissue healing, increase tissue extensibility, modify skin and scar tissue, and decrease edema/inflammation.
PAMs are used in preparation for or concurrently with purposeful and occupation-based activities.
PAMs are categorized as preparatory methods (AOTA, 2002) that also can be used concurrently with purposeful activity or during occupational engagement. Preparatory methods support and promote the acquisition of the performance skills necessary to enable an individual to resume or assume habits, routines, and roles for engagement in occupation. The exclusive use of PAMs as a therapeutic intervention without application to occupational performance is not considered occupational therapy. When used, PAMs are always integrated into a broader occupational therapy program as a preparatory method for the therapeutic use of occupations or purposeful activities.
Categories of physical agents include:
1. Superficial thermal agents
2. Deep thermal agents
3. Electrotherapeutic agents
4. Mechanical devices
5. Light therapy
1. Superficial Thermal Agents
Hydrotherapy/whirlpool, cryotherapy (cold packs, ice), Fluidotherapy,™ hot packs, paraffin, water, infrared, and other commercially available superficial heating and cooling technologies.
a. Superficial Heat
In contrast to deep heating modalities, superficial heating modalities usually do not heat deep tissues, including muscles, because the subcutaneous layer of fat beneath the skin surface acts as a thermal insulator and inhibits heat transfer.
The transfer of heat can be classified into 3 general types of heat transfer: conduction, convection, and conversion.
I. Conductive heating – This is defined as heat transfer from one point to another without noticeable movement in the conducting medium; typically, direct contact takes place between the heat source and the target tissues; superficial heat is usually conductive heat for example: hot water baths, hot packs, paraffin baths
II. Convective heating – This form of heating is produced by the movement of the transferring heating medium, usually air or a fluid; methods for providing convective superficial heat include Fluidotherapy and whirlpool
III. Conversion heating – This involves the conversion of one energy form (eg, light, sound) into another (heat); superficial heat is produced by heat lamps or radiant light bakers, with heat being transferred when the conveying medium (light energy) is converted to heat energy at the skin surface.
b. Therapeutic Cold (Cryotherapy)
Cryotherapy has the primary effect of cooling tissue. Depending upon the application method and duration of this therapy, the basic physiologic effects include the following:
• Decreased local metabolism
• Vasoconstriction
• Reactive hyperemia
• Reduced swelling/edema
• Decreased hemorrhage
• Reduced muscle efficiency
• Analgesia secondary to impaired neuromuscular transmission
• Pain reduction associated with the application of cold, which relaxes muscle spasm and minimizes upper motor neuron spasticity
2. Deep Thermal Agents
Therapeutic ultrasound, phonophoresis, short-wave diathermy, and other commercially available technologies.
Deep heat is produced when energy is converted into heat as it passes through body tissues.
Energy sources include the following:
I. High-frequency currents (shortwave diathermy)
II. Very-high-frequency electromagnetic radiation (microwave diathermy)
III. High-frequency sound (ultrasound diathermy)
The temperature distribution in the tissues heated by any of these modalities results from the pattern of relative heating, which is the amount of energy converted to heat at any given location. The physiologic effects of temperature occur at the site of the application and in distant tissue. The local effects are caused by the elevated temperature response of cellular function by direct and reflex action. Locally, there is a rise in blood flow with associated capillary dilatation and increased capillary permeability. Initial tissue metabolism increases, and there may be changes in the pain threshold. Distant changes from the heated target location include reflex vasodilatation and a reduction in muscle spasm (as a result of skeletal muscle relaxation).
3. Electrotherapeutic Agents
This modality uses electricity to stimulate nerves or muscles via electrodes. Electricity and the electromagnetic spectrum are used to facilitate tissue healing, improve muscle strength and endurance, decrease edema, modulate pain, decrease the inflammatory process, and modify the healing process.
Electrotherapeutic agents include neuromuscular electrical stimulation (NMES), functional electrical stimulation (FES), transcutaneous electrical nerve stimulation (TENS), interferential therapy (IFT), high-voltage galvanic stimulation for tissue and wound repair, iontophoresis, and other commercially available technologies.
General Guidelines:
Electrical stimulation (all forms) should not be applied:
• To areas where it could cause malfunction of electronic devices, including cardiac pacemakers
• To the lower back or abdomen of pregnant women
• To acupuncture points of pregnant women
• To regions of known or suspected malignancy
• To persons with active deep vein thrombosis or thrombophlebitis
• To actively bleeding tissue or to persons with untreated hemorrhagic disorders
• To infected tissues, tuberculosis, or wounds with underlying osteomyelitis
• To recently radiated tissues
• To the chest in persons with cardiac disease, arrhythmias, or heart failure
• To the neck or head region of persons known to have seizures
• To areas near reproductive organs or genitalia without specialized training
• To areas near or over eyes
• To anterior neck or carotid sinus
• To damaged or at-risk skin areas that would result in uneven conduction of current (excluding open wounds where the specific intent is to use electrical stimulation for tissue healing)
Electrical stimulation (all forms) can be applied with caution to:
• Active epiphysis
• Persons with skin diseases (e.g., eczema, psoriasis)
Electrical stimulation (all forms) can be used on:
• Intact skin overlying implants containing metal, plastic, or cement
• Tissues inflamed as a result of recent injury or exacerbation of a chronic inflammatory condition
Spinal traction, vasopneumatic devices and continuous passive motion (CPM) are commonly used examples.
5. Light therapy
Low level energy Laser therapy (LLLT) uses low-powered laser light to produce a biological response in tissue.
Mechanism of action: It does not produce a thermal effect. It is proposed to affect fibroblast function and accelerate connective tissue repair. Some research suggests LLLT has an anti-inflammatory effect by reducing prostaglandin synthesis.
Indications: It is commonly used to decrease acute and chronic pain and inflammation, stimulate collagen metabolism and promote wound healing.
Contraindications and precautions: Treatment over malignancy, irradiation of the neck region in hyperhidrosis, epilepsy, exposure of the retina, and exposure of the abdomen during pregnancy
PAMs may only be applied by OTs and OTAs who have documented evidence of possessing the theoretical background and technical skills for safe and competent integration of the modality into the occupational therapy plan.
| Physical Agent Modality | Description | Indications | Administration Techniques | Precautions/Contraindications |
| Cryotherapy /Cold pack
Superficial Thermal Agent
|
Cold
Physiologic effects of cold: decreases pain, blood flow, edema, inflammation, muscle spasm, and metabolic demand |
Used for pain management, anti inflammation, edema control, decrease of muscle guarding, spasm.
-Cold therapy should be the modality of choice in the acute state following trauma. Cold may be uncomfortable at first but pain, edema, inflammation and muscle spasm will ultimately be reduced. -Cold is often used in conjunction with rest compression and elevation. RICE – Rest, Ice, Compression, Elevation -Cold in combination with static stretch or contract relax technique has been recommended for reducing muscle spasm or decreasing exercise induced muscle soreness thus increasing ROM. |
Cooling agents include: Cold packs, ice massage, cold baths, vapocoolant spray, cold gel, controlled cold compression units | • Hypersensitivity or poor tolerance to cold • Raynaud’s disease and phenomenon** • Circulatory impairment – e.g. hemorrhaging tissue or untreated hemorrhagic disorders • Peripheral vascular disease • Active DVT • Impaired sensation (neuropathy) • Open wounds, near chronic wounds • Cryoglobulinemia*** • Over regenerating nerves • Impaired cognition and/or ability to communicate .. *** Cryoglobulinemia is a disorder characterized by the presence of an abnormal blood protein that forms a gel when exposed to low temps. This gel formation can lead to ischemia or gangrene. .. ** Raynaud’s phenomenon is a vasospastic (a sudden constriction of a blood vessel that reduces blood flow) disorder that is idiopathic (a disease that has no known cause) or associated with other disorders. Cycles of pallor, cyanosis, rubor, numbness, tingling or burning. |
| Superficial Heat
Superficial Thermal Agent
|
Hot Physiologic effects of heat: pain relief, increase in local blood flow, metabolism and elasticity of connective tissues. ** Heat increases bleeding and edema and may exacerbate acute inflammation.
|
Heat is usually used for subacute and chronic conditions. Relieves pain, increases soft tissue extensibility, reduces muscle spasm, relaxes skeletal muscles, decreases joint stiffness, and promotes wound healing. |
Commonly used superficial heat modalities include: hot packs, heating pads, paraffin bath, infrared and fluidotherapy.
PAM must benefit the patient. Used as adjunctive intervention in preparation for purposeful, functional activity. |
• Peripheral vascular disease • Impaired circulation, bleeding disorder, DVT or thrombophlebitis • Local malignancy and recently radiated areas • Acute inflammation or trauma, edema, infection • Open wounds • Over large scars • Impaired sensation (neuropathy) • Large areas, or at sufficient intensity to raise core temperature- pregnancy, severe cardiac disease/in cardiac failure • Impaired ability to communicate- cognition or communication impairments sufficient to prevent patient from giving accurate and timely feedback • Areas affected by heat-sensitive skin diseases (e.g., eczema) • Areas of skin breakdown or damage producing uneven heat conduction across the skin • Reproductive organs (testes) |
| Fluidotherapy
Superficial Thermal Agent
|
Superficial heating modality that transfers heat by convection. Dried corn husks or other cellulose material are suspended by warmed circulating air | Mainly used to help patients with their hands and wrists. Arthritis, chronic tendonitis, postoperative conditions, post fracture management, and Raynaud’s syndrome. | The machine is heated to desired temperature, then the distal limb is placed inside the fluidotherapy cabinet. Turbulence of the suspended particles can be controlled. Treatment time is typically 15-20 minutes. | Open wounds- Open wounds must be covered with a plastic barrier to prevent cellulose particles from entering the wound.
General contraindications for Superficial Heat also apply |
| Interferential Current (IFC)
Electrotherapeutic Agent
|
IFC uses two wave kilohertz frequencies and creates an interference between them, resulting in a unique current | Used for pain management, edema reduction, and muscle spasm reduction. | Uses four electrodes set up so that the two wave currents intersect one another perpendicularly. Intensity is increased to patients tolerance. Patients should feel a comfortable tingling sensation. | • Electrodes should not intersect thoracic cavity • Contraindicated during pregnancy • Presence of a cardiac pacemaker, or other implanted electrical simulators • Cancer due to risk of metastasis • Hemorrhaging tissue • Thrombosis Precautions include obesity, impaired sensation, over superficial implants, and impaired cognitive abilities. General contraindications for electrical stimulation also apply |
| Iontophoresis
Electrotherapeutic Agent
|
A continuous direct current used to transmit ions through the skin. | Used for pain management, anti inflammation, scar lysis, and enhanced healing. The specific medication that is used in iontophoresis depends upon the goals of treatment. Chlorine is a negatively charged ion used in iontophoresis in the treatment of scar tissue and keloid scars. | Uses two electrodes; one active and one dispersive. Best applied to a specific, localized, and relatively superficial target tissue. Such tendons include the rotator cuff tendons, common wrist/finger/hand flexor and extensor origins. | • Areas with bruises • Areas with cuts, broken skin • Acute injuries • Impaired sensation • Over sites of active hemorrhage General contraindications for electrical stimulation also apply |
| Neuromuscular Electrical Stimulation (NMES)
Electrotherapeutic Agent
|
Therapeutic muscle stimulation: repetitive simulation to paralyzed muscle to minimize atrophy and maintain range of motion. Activate muscle by stimulating an intact or partially intact peripheral nerve. | Used to stimulate paralyzed, paretic muscle, muscle weakness, peripheral neuropathy, and muscle spasm. | Pulse amplitude is gradually increased within the patients sensory tolerance limits. | • Pregnancy • Cancer • Presence of a cardiac pacemaker, or any other electrical simulators. Precautions include obesity, impaired sensation, and over relatively superficial metal implants. General contraindications for electrical stimulation also apply |
| Paraffin baths
Superficial Thermal Agent
|
Superficial heat by coating the target area with solution with melted paraffin wax and mineral oil. | A paraffin bath is a form of conductive heating. Paraffin baths are particularly useful for contractures due to rheumatoid arthritis, burns, and progressive systemic sclerosis (scleroderma). Used to treat chronic arthritis of the hand, various distal extremity conditions to increase ROM, manages pain, and assists in wound healing.
Most commonly used for distal extremities |
Dip technique-the distal extremity is coated with 8 to 12 coats of paraffin. Then the distal extremity is wrapped in plastic and then a terry towel. The patient is positioned so the extremity is elevated. The paraffin glove remains in place for 15 to 20 minutes. | Contraindicated if patient has open wounds, abrasions or skin infections.
General contraindications for Superficial Heat also apply |
| Transcutaneous Electrical Nerve Stimulation (TENS)
Electrotherapeutic Agent
|
Used to stimulate sensory and/or motor nerves in an effort to manage pain. | Stimulates nerve fibers and provides symptomatic relief of pain. Used to treat chronic pain syndrome, spinal radiculopathy, low back pain, reflex sympathetic dystrophy, etc. TENS has been found be effective in treating neuropathic pain is spinal cord injury patients and painful diabetic peripheral polyneuropathy. |
Uses high pulse rate and low pulse width. Patients should be allowed to ambulate, perform ADL’s, and occupational tasks while the modality is administered. | • Pregnancy • Pacemakers • Prone to seizures- Tens “pulses” have the potential to trigger a seizure. General contraindications for electrical stimulation also apply |
| Ultrasound
Deep Thermal Agent
|
Deep heating modality. Sound waves are extremely low intensity and very high frequency are introduced to tissue, producing thermal and non-thermal effect. | Penetrates deep into the musculature and joint tissues. • Increase the extensibility of collagen fibers in tendons and joint capsules • Reduce muscle spasms • Aids tissue healing – speeds up the rate of healing & enhance the quality of the repair • Modulate pain, goes to the deepest layer for pain |
Conducting gel is required.
Mode: continuous vs pulsed. Continued US provides mainly thermal effects while pulsed US emphasizes nonthermal effect |
• Pacemaker • Areas of decreased circulation • Impaired sensation • Pregnancy • Along the cervical sympathetic ganglion (or over the anterolateral neck) • Directly over the spinal column after laminectomy • Severe arterial disease or DVT • Bleeding disorders • Over a bony prominence • Over epiphyseal plates • Any surgically implanted artificial product (e.g., Gortex or mesh) may build up heat in an area. ** While recent research shows some promise for ultrasound as an effective treatment to accelerate healing of fractures, AOTA’s official stance is that ultrasound is contraindicated for fractures. |
| Whirlpool
Superficial Thermal Agent
|
One of the oldest types of hydrotherapy. The principle of whirlpool therapy is to combine the effects of temperature with the mechanical effects of water.
|
Whirlpools are used for delivering heat or cold for: • Pain management • Wound management, particularly in the management of burn patients • To facilitate debridement in infected wounds, non-draining wounds, wounds with thick eschar, and on wounds with loosely adherent necrotic tissue • Helps dressings to be removed slowly and gently, reducing the pain of dressing changes. • ROM exercises • Promoting muscular relaxation |
Whirlpools consist of a large or small tank filled with water. The temperature of the water in the whirlpool can be warm or cold, depending on the desired goal. The water temperature is generally set between 100°–104° F, however, if a patient is heat-sensitive, a burn victim, or a child, the temperature is usually lessened to 96°–98° F. The body part that is to be treated is then placed in the tub of water, and a small motor agitates the water. The motor on the whirlpool provides air bubbles causing water turbulence. The turbulence can be graded from limited to full turbulence. | • Fever • Recent skin grafts • Circulatory impairment • Active bleeding/ hemorrhaging • Open wounds • Sensory or vascular impairment .. General contraindications for Superficial Heat and Cold also apply |
| Contrast baths
Superficial Thermal Agent
|
The theory of contrast bath use is to create a rapid opening and closing of the arteries around the body part being treated. This creates a pumping effect in the body part, which helps to decrease swelling around the injured site. | Hot/cold immersion therapy is a method of treating: • Muscle soreness • Swelling • Inflammation. • Joint injuries, mild sprains, • Symptoms of chronic pain and repetitive strain injuries • Edema |
A contrast bath treatment involves using both warm and cold on the same body part during treatment. The injured body part is repeatedly moved from the warm to cold water | Same as Superficial Heat and Cold |
PAM PRECAUTIONS – quick reference
| Cold Therapy | Hot Therapy | Interferential | TENS | Ultrasound | Paraffin Wax | |
| Active Epiphysis |  |
 |
 |
 |
 |
 |
| DVT |  |
 |
 |
 |
 |
 |
| Local Circulatory Insufficiency |  |
 |
 |
 |
 |
 |
| Malignancy |  |
 |
 |
 |
 |
 |
| Metal Implant |  |
 |
 |
 |
 |
 |
| Pacemaker |  |
 |
 |
 |
 |
 |
| Pregnancy |  |
 |
 |
 |
 |
 |
![]()
No precautions or contraindications

Take precautions

Contraindicated
Resources:
https://emedicine.medscape.com/article/1833084-overview
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3031347/#__sec219title
http://samples.jbpub.com/9781449653415/53415_CH02_Sample.pdf
https://uw.cloud-cme.com/assets/uw/Presentations/1129/Sun_1100_McGough.pdf