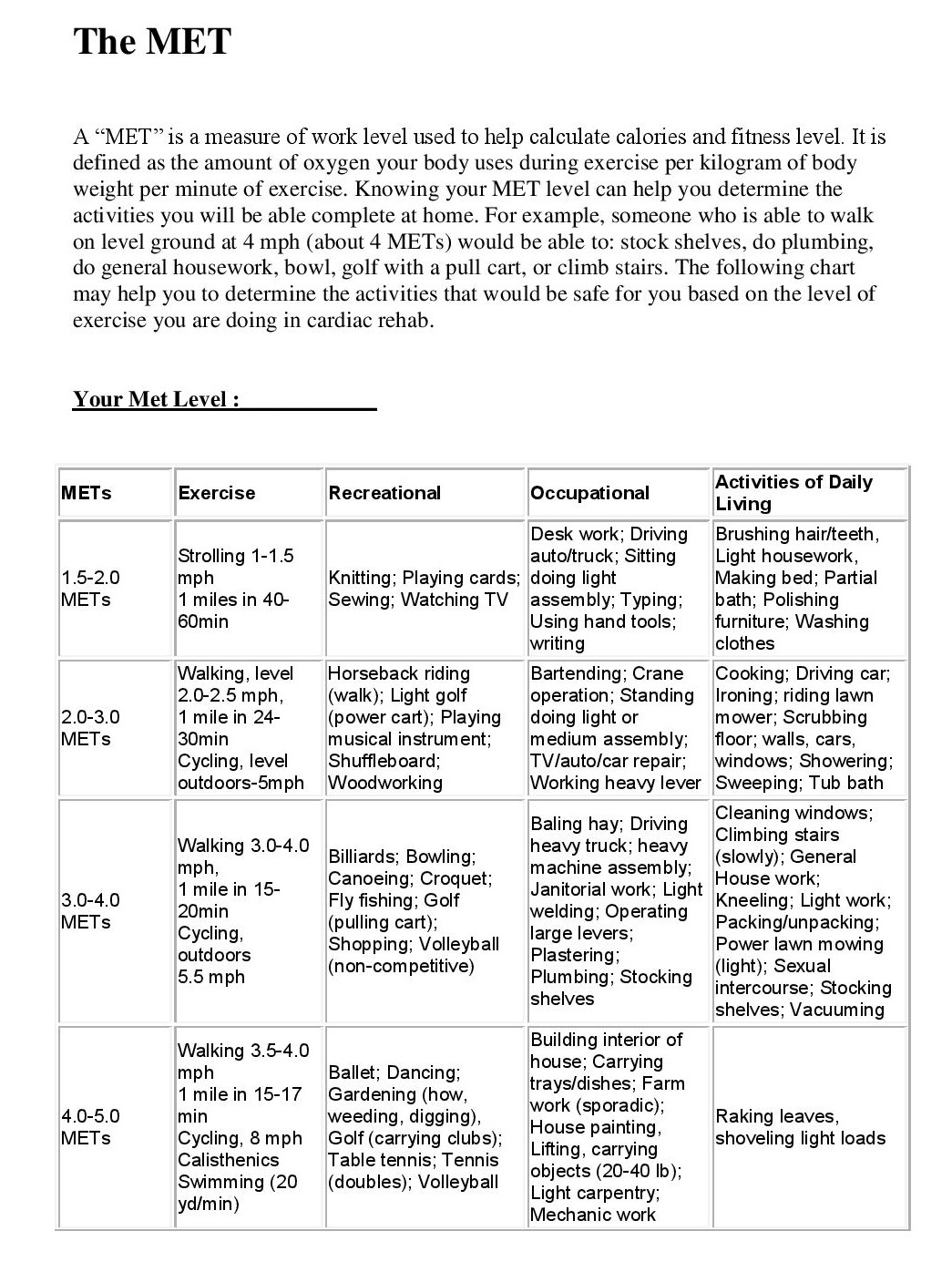
The Metabolic Equivalent of Task, or MET level, is the approximate amount of energy a person uses during physical activity. These levels are used as a reference point during cardiac rehabilitation. Patients who have had a heart attack or who have undergone open heart surgery are assisted to gradually return to normal activity levels, using MET levels as a guide to insure that activity does not exceed what the patient’s heart can tolerate. Following are some guides to help you learn the stages of cardiac rehabilitation, as guided by MET levels.
This system is used to classify heart disease according to the activity level that patients can tolerate.
| Class | Patient Symptoms | Approximate MET Level Tolerated |
| I | No limitations. Patients do not experience heart palpitations, shortness of breath, or extreme fatigue during normal physical activity. | 4.5 and over |
| II | Slight limitations of physical activity. Patients are comfortable at rest. Ordinary physical activity results in palpitations, shortness of breath, or fatigue. | Up to 4.5 |
| III | Significant limitations of physical activity. Patients are comfortable at rest. Light to moderate activity causes palpitations, shortness of breath and fatigue. | Up to 3.0 |
| IV | Unable to tolerate physical activity. Patients experience palpitations, shortness of breath and fatigue even at rest. Physical activity increases the severity of symptoms. | Up to 1.5 |
These are the stages used during cardiac rehabilitation to present activities to patients.
MET levels are used to ensure that the activities do not exceed the patient’s activity tolerance.
| Stage | MET Level Range | ADL Restrictions | Recreational Restrictions | Exercise Restrictions | Pictures |
| I | 1.0 – 1.4 | Sitting up is allowed for short periods. Self-feeding, washing hands and face, bed mobility, transfers. | Sitting: Reading, radio, non-competitive table games, light handwork. | Can exercise all extremities in supine (10-15x, at a time). Can only sit to exercise neck and lower extremities. |  |
| II | 1.4 – 2.0 | Sitting up is allowed as tolerated – no limitations to sitting. Sitting: Self-bathing, shaving, dressing, grooming. |
Sitting: Crafts, painting, knitting, sewing, mosaics, embroidery. | May exercise all extremities but NO ISOMETRICS or strengthening exercises are allowed. AROM to all extremities, progressively increasing number of repetitions.
Walking at slow pace in room, as tolerated |
 |
| III | 2.0 – 3.0 | Sitting: Showering in warm water.
Sitting: Ironing, housekeeping tasks with brief standing periods to transfer light items. |
Sitting: card playing, crafts, piano, machine sewing, typing. | Sitting: wheelchair mobility limited distances Standing: AROM exercises to all extremities, progressively increasing number of reps. May include: balance exercises, light mat work with no resistance Walking on a zero gradient and comfortable pace is allowed. |
 |
| IV | 3.0 – 3.5 | Standing: showering in warm water, self, dressing, shaving, grooming,
Light housekeeping tasks while standing, using energy conservation – light vacuuming, dusting, sweeping, washing light clothing. |
Bowling, slow canoeing, golf putting, light gardening -planting, driving. | Standing: all previous exercise, progressively increasing number of reps and speed. May include balance and mat exercises with light resistance.
Walking: unlimited, zero gradient, progressing speed/duration for up to 15-20 min or target HR reached. May begin walking on a treadmill at 1 to 1.5 mph, at a 1-2% grade. |
 |
| V | 3.5 – 4.0 | Standing: washing dishes, washing clothes, ironing, hanging light clothes, making beds. | Slow swimming, light carpentry, golfing, light home repairs. |
Sitting: More resistance may be added to exercises completed while sitting, up to 10 lbs.
Standing: continue with previous exercises, progressively increasing number of reps and speed. Walking: Unlimited, increasing speed up to 2.5mph, on level surfaces. Stairs: Increase tolerance. Cycling: up to 8 mph with no resistance. |
 |
| VI | 4.0 and above | Standing: showering in hot water, hanging/wringing clothes, mopping, stripping and making beds, raking. | Swimming-no advanced strokes, slow dancing, slow ice or roller skating, volleyball, badminton, table tennis, light calisthenics. | Sitting: Exercising upper and lower extremities, up to 10-15 lbs.
Walking: increase speed to 3.5 mph. Cycling up to 10 mph, no resistance. |
 |
These phases are used as a basic protocol when providing cardiac rehabilitation services to patients.
Phase I: This phase begins during the patient’s inpatient hospital stay. It usually continues for up to 14 days after the patient’s initial procedure or cardiac event.
| MET Level | Precautions | Activities | Monitoring |
| Begins at MET level 1-2 Target MET level 3.5 |
No isometric exercises or muscle strengthening work
No overhead or lateral upper body activity |
Patient education in the following areas: ● Energy conservation ● Work simplification ● Risk factors ● Smoking cessation Light activity if regular pulse is 100 bpm or less |
Take vital signs (blood pressure, pulse, respiration) at the beginning of each activity, at the peak of each activity, at the end of each activity, and 4-5 minutes after each activity.
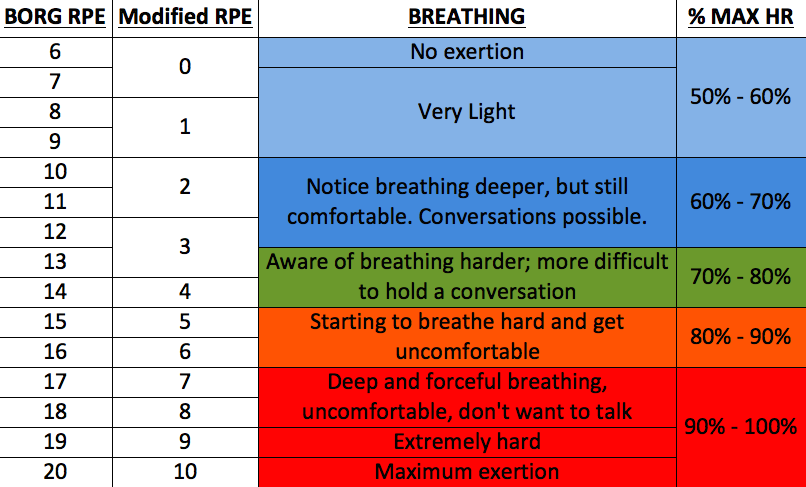
May use a perceived exertion scale to monitor the patient’s perception of effort. (example – BORG scale for exertion) |
.
Phase II: This phase begins when a patient is able to tolerate an activity level at 3.5 MET. It is completed through outpatient rehabilitation and can last up to 12 to 18 weeks after the patient’s initial cardiac event.
| MET Level | Precautions | Activities | Monitoring |
| Begins at MET level 4-5
Target MET level 5-6 |
Build up activity tolerance gradually
May start graded weight training 2-4 weeks after the initial cardiac event |
Continued patient education as in Phase I
Practice work simplification and energy conservation techniques Gradual graded exercise Gradual graded weight training Home evaluation Work site evaluation if applicable May be referred to a work hardening program if needed |
Continued monitoring of vital signs during and after activity
May use perceived exertion scale. Target for BORG scale 11-15. |
.
Phase III: This phase of cardiac rehabilitation involves maintenance of the gains made in phases I and II. It may begin as early as 4 weeks after the initial cardiac event, depending on the patient.
Phase III cardiac rehabilitation programs are usually provided in community exercise facilities, such as the YMCA. A physician must refer a patient to a Phase III cardiac rehabilitation program. Since these programs are community based, insurance may not cover the cost.
| MET Level | Precautions | Activities | Monitoring |
| Begins at MET level 5-6 | Patient is educated in precautions and self monitors during activity. | Maintenance gym exercise program
Weight training Cardiovascular exercise |
Patient usually undergoes a stress test prior to participating in the program. |

…
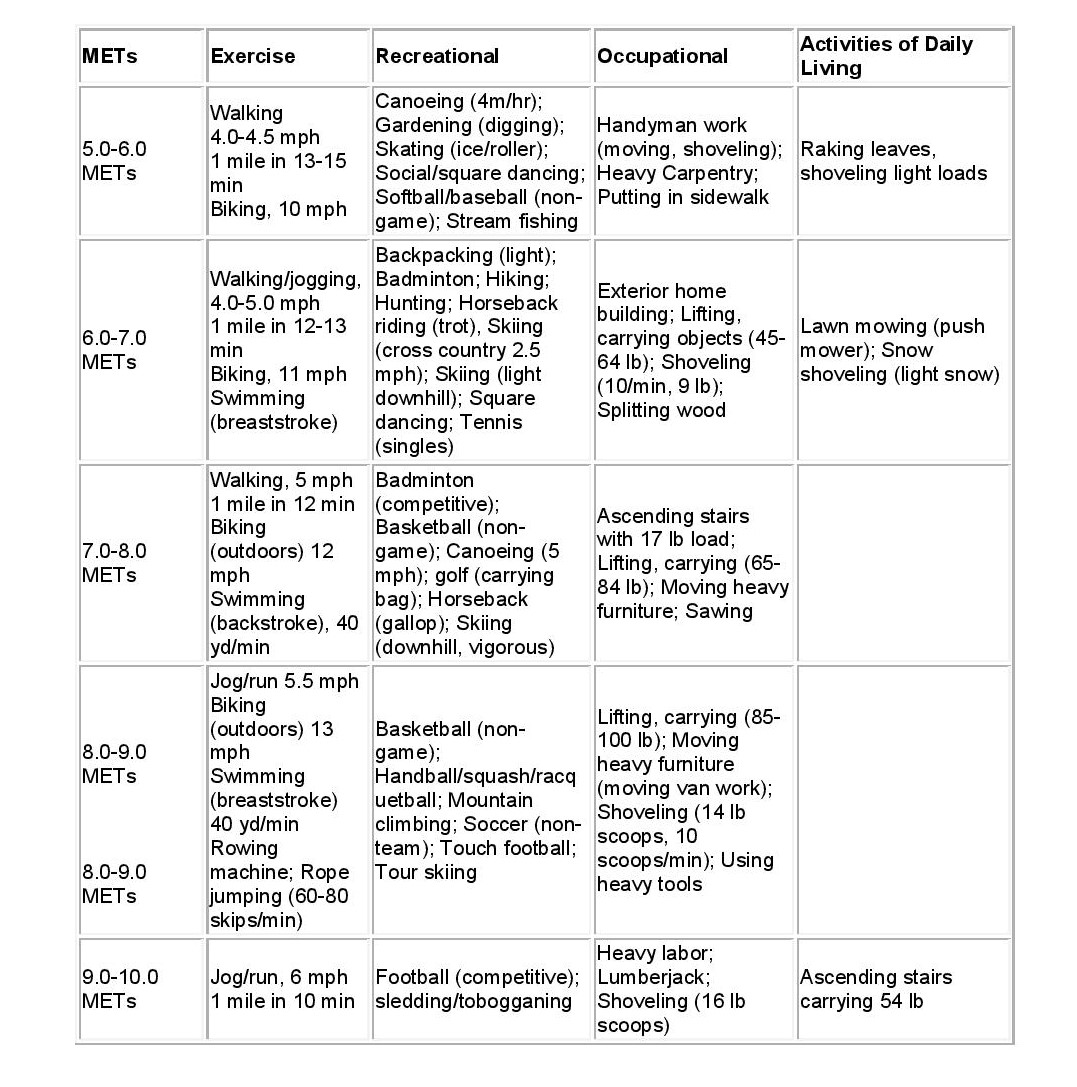
Reference: https://www.bronsonhealth.com/app/files/public/744/BronsonCardiaRehabHomeExerciseBook.pdf
![]() 2011 Compendium of Physical Activities
2011 Compendium of Physical Activities
The Compendium of Physical Activities was developed to enhance the comparability of results across studies using self-report physical activity (PA) and is used to quantify the energy cost of a wide variety of PA. The 2011 Compendium retains the previous coding scheme to identify the major category headings and specific PA by their rate of energy expenditure in MET values. The Compendium is used globally to quantify the energy cost of PA in adults for surveillance activities, research studies, and, in clinical settings, to write PA recommendations and to assess energy expenditure in individuals. The 2011 Compendium is an update of a system for quantifying the energy cost of adult human PA and is a living document that is moving in the direction of being 100% evidence based.
Follow this link to download/view the compendium.
http://download.lww.com/wolterskluwer_vitalstream_com/permalink/mss/a/mss_43_8_2011_06_13_ainsworth_202093_sdc1.pdf
| Infant 0-12 months | Child 1-11 years | Teen to Adult Over age 12 | |
| Blood pressure | 65-90/45-65 0-6 months, 80-100/55-65 6-12 months | 90-110/55-75 | 110-135/65-85 |
| Pulse (beats per minute) | 100-160 bpm | 70-120 bpm | 60-100 bpm |
| Respiration | 30-60 breaths/minute 0-6 months; 24-30 breaths/minute 6-12 months |
20-30 breaths/minute 1-5 years; 12-20 breaths/minute 6-12 years |
12-18 breaths/minute |
Borg Scale of Perceived Exertion
| Patient’s description of exertion | Borg rating | Example of activity |
| None | 6 | Reading, watching TV |
| Very, very light | 7-8 | Tying shoes, writing |
| Very light | 9-10 | Folding laundry |
| Fairly light | 11-12 | Walking, shopping |
| Somewhat hard | 13-14 | Brisk walking, vacuuming or cleaning |
| Hard | 15-16 | Swimming, bicycling |
| Very hard | 17-18 | Highest level of sustainable activity |
| Very, very hard | 19-20 | A burst of activity that cannot be sustained for a long time. |